CASE
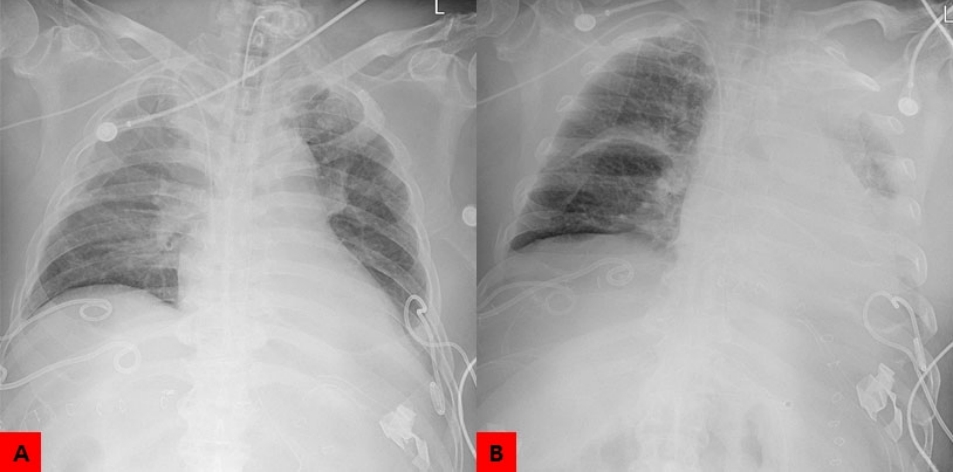
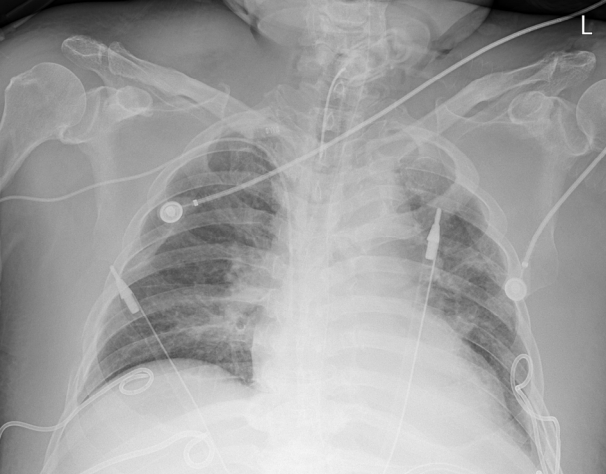
A 66-year-old male presented to the emergency department after suffering a major trauma. Endotracheal intubation and ventilator care were initiated on day 6 after hospitalization due to severe dyspnea. Open tracheostomy was performed on the 14th day of intubation. On the 20th day of tracheostomy, no atelectasis was observed in the AP chest radiography (Fig. 1A) and ABGA revealed the pH of 7.37, pCO2 of 36, pO2 of 121, HCO3− of 20.8, and O2 sat of 98.1. However, the total atelectasis in the left lung was observed in the AP chest radiography performed on the following day (Fig. 1B) and ABGA deteriorated to pH of 7.30, pCO2 of 42, pO2 of 54, HCO3− of 20.7, and O2 sat of 86.9. Fiberoptic bronchoscopy was performed to flush a very large amount of thick purulent secretion that totally obstructed the left main bronchus (Fig. 2). Atelectasis disappeared in the follow-up AP chest radiography (Fig. 3) and ABGA improved to pH of 7.32, pCO2 of 42, pO2 of 113, HCO3− of 21.6, and O2 sat of 99.2.
DISCUSSION
Atelectasis is a state in which the lungs are completely or partly collapsed, most commonly occurs postoperatively, and is caused by cystic fibrosis, lung tumors, chest injuries, lung fluids, respiratory weakness, and presence of foreign objects. Mucous plugs can also lead to atelectasis, and the main broncheal plug leads to complete pulmonary collapse, which can ultimately lead to life-threatening conditions [1]. Conventional chest radiography in a critically ill patient is the cornerstone of day-to-day management [2]. In addition, the possibility of atelectasis should be considered when O2 sat and pO2 changes occur. In this case, following a bronchoscopic toilet, O2 sat decreased from 98.1 to 86.9 and then increased to 99.2, whereas pO2 decreased from 121 to 54, and then increased to 113. Ghosh et al. [3] reported a case of left main bronchus obstructed by a chunk of thick mucous in a 6-year-old male, and a uniform opacity involving the whole lung field obscuring the heart shadow (Silhouette sign).