|
 |
- Search
| Trauma Image and Procedure > Volume 2(1); 2017 > Article |
|
Abstract
We report a case of damage control surgery (DCS) performed for abdominal compartment syndrome (ACS) due to delayed rupture of hepatic subcapsular hematoma, confirmed by initial abdominal computed tomography (CT) after blunt trauma. A 58-year-old man presented to the emergency department with a Glasgow Coma Scale Score 5 after a passenger traffic accident. Abdominal CT demonstrated a large crescent-shaped hepatic subcapsular hematoma (10 x 5 x 17 cm in size). During neurosurgery, ACS developed due to delayed rupture of a subcapsular hematoma and DCS was performed. Immediately after temporary abdomen closure (TAC), the patient was transferred to the intervention room and transcatheter arterial embolization (TAE) was performed on the bleeding site from the liver surface. Two days after surgery, gauze removal and definitive closure of the abdomen were performed. The patient was transferred to the rehabilitation department 4 weeks postoperatively.
A 58-year-old man presented to the emergency department with a Glasgow Coma Scale Score 5 after a passenger traffic accident. His vital signs were blood pressure 110/60 mmHg, pulse rate 118 beats/min, respiration rate 27 breaths/min, body temperature 36.6Ōäā, and oxygen saturation 99%. The Injury Severity Score (ISS) was 43, revised trauma score (RTS) was 5.03, and trauma and injury severity score (TRISS) was 15.2%. Laboratory examination revealed white blood cell count (WBC) 7.52 ├Ś 103 /╬╝L, hemoglobin (Hb) 11.0 g/dL, platelet 39 ├Ś 103 /╬╝/, lactic acid 3.8 mmol/L, and base excess -6.6. Abdominal computed tomography (CT) demonstrated a large crescent-shaped subcapsular hematoma of the right hepatic lobe (segments 5ŌĆō8) without a definite parenchymal laceration. The subcapsular hematoma was 10 ├Ś 5 ├Ś 17 cm in size and was not ruptured. Contrast leakage was observed at the parenchymal boundary (Fig. 1., 2.). The brain showed severe subdural hematoma (SDH), extradural hematoma (EDH), and intracerebral hemorrhage (ICH), and emergency craniotomy was performed. During surgery, systolic blood pressure decreased to less than 90 mmHg, heart rate increased to more than 120 beats/min, and abdominal distension became prominent. In the operating room, intra-abdominal ongoing hemorrhage accompanied by abdominal compartment syndrome (ACS) was suspected and emergency laparotomy was performed. A large amount of hematoma of more than 3 L was observed in the abdominal cavity at laparotomy and 4-quadrant gauze packing was performed. A capsule of hepatic subcapsular hematoma was ruptured, causing ongoing bleeding from the ruptured hematoma. In addition, severe intestinal edema was noted (Fig. 3.). After contacting the interventional radiologist for transcatheter arterial embolization (TAE), we performed damage control surgery (DCS). A perihepatic packing and temporary abdomen closure (TAC) was performed (Fig. 4.). Immediately after the operation, TAE was performed for the bleeding arteries from the ruptured hematoma (Fig. 5.). The patient was admitted to the trauma intensive care unit (TICU) and his physiologic status improved. Two days postoperatively, gauze removal and definitive closure of the abdomen were performed. The ruptured hematoma decreased gradually over time (Fig. 6.). The patient was transferred to the rehabilitation department 4 weeks postoperatively.
Hepatic subcapsular hematoma caused by blunt trauma is not a rare condition. However an unruptured large subcapsular hematoma is rare. Taff et al. [1] reported a case of sudden death due to delayed rupture of a hepatic subcapsular hematoma. The possibility of rupture should be considered when the size of the supcapsular hematoma is large as in this case. In patients with large hepatic subcapsular hematoma rupture, if bleeding control is difficult or coagulopathy progresses, TAE after DCS also can be a treatment option [2,3]
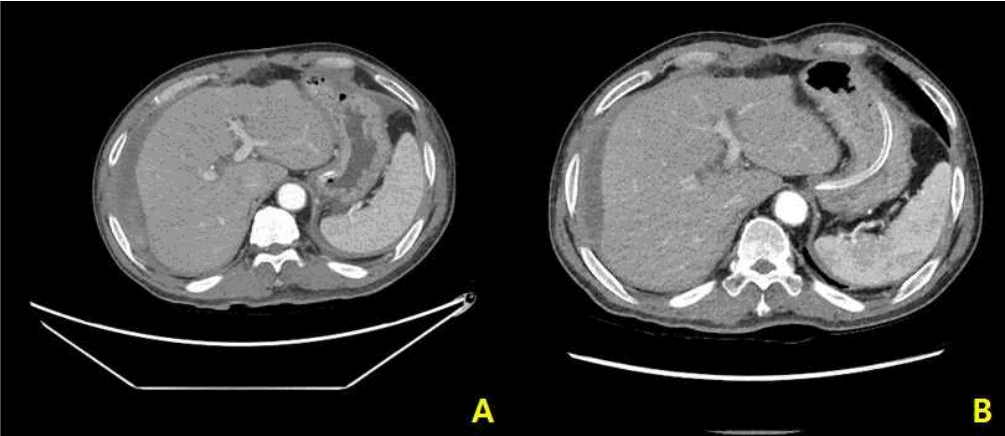
Fig.┬Ā1.
Abdominal CT (axial view) demonstrates a large crescent-shaped subcapsular hematoma of the right hepatic lobe without a definite parenchymal laceration. The subcapsular hematoma was not ruptured. Contrast leakage was observed at the parenchymal boundary.

Fig.┬Ā2.
Abdominal CT (coronal view) demonstrates a large crescent-shaped subcapsular hematoma of the right hepatic lobe without a definite parenchymal laceration. The subcapsular hematoma was not ruptured. Contrast leakage was observed at the parenchymal boundary.
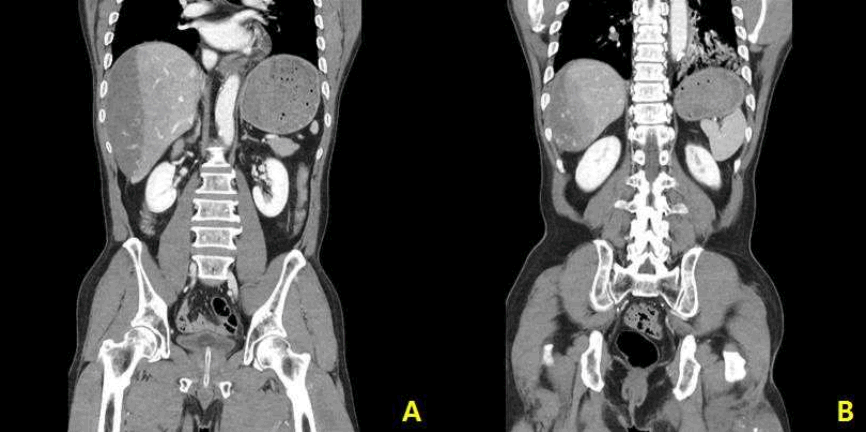
Fig.┬Ā3.
The abdomen was severely distended during craniotomy (A). A capsule of hepatic subcapsular hematoma was ruptured, causing diffuse bleeding from the liver surface. A severe intestinal edema was also noted (B).
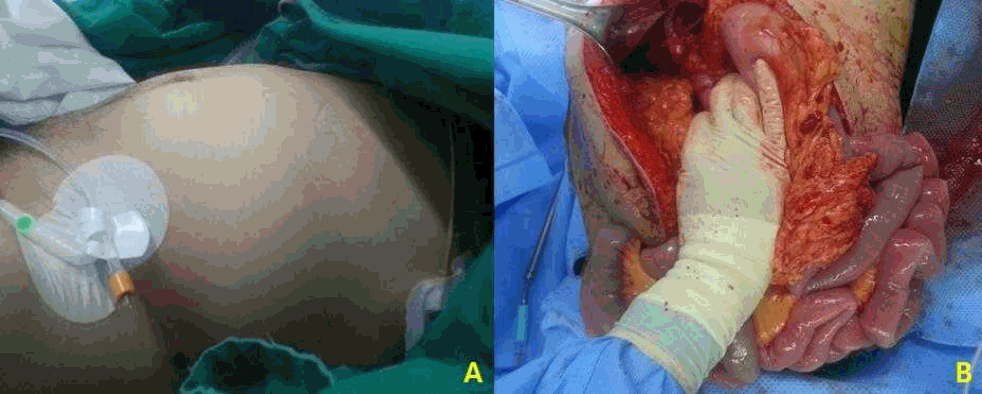
Fig.┬Ā4.
A perihepatic packing was performed, two 4-layered gauzes were placed between the liver and lateral abdominal wall (one on segments 5 and 6, another on segments 7 and 8) and the abdominal wound was closed temporarily.

REFERENCES
1. Taff ML, Wolodzko AA, Boglioli LR. Sudden death due to delayed rupture of hepatic subcapsular hematoma following blunt abdominal trauma. The American journal of forensic medicine and pathology. 1990;11(3):270.