Inappropriate Resuscitative endovascular balloon occlusion of the aorta (REBOA) Catheter Placement in Patient With Unexpected Left Common Iliac Artery Rupture
Article information
Abstract
Resuscitative endovascular balloon occlusion of the aorta (REBOA) is effective method increasingly used in cases of traumatic noncompressible torso hemorrhage. However, it is performed in an emergency situation, and the source of hemorrhage cannot be verified during implementation, which may make it difficult to place the catheter accurately.
In the case reported here, catheter placement was inappropriate.
CASE
A 70-year-old man came to our facility after a car accident. The vital signs were unstable; blood pressure could not be recorded at the time of arrival. Immediately after arrival, cardiac arrest occurred twice, and resuscitation was successful. In the emergency room, he underwent brief sonographic examination, and a massive fluid collection was observed in the splenorenal recess. Resuscitative endovascular balloon occlusion of the aorta (REBOA) was also performed with blind puncture technique during the resuscitation. The balloon was inflated with 25 mL of normal saline, but there was no sense of resistance, which is considered unusual. Placement of the catheter tip was checked with bedside ultrasonography but was not clearly confirmed because of the massive fluid collection. In general, catheter tip placement is confirmed with radiography, fluoroscopy, or ultrasonography [1], but the serious emergency situation precluded these assessments. The patient’s blood pressure recovered to 80/50 mm Hg, and he was moved to the operating room immediately.
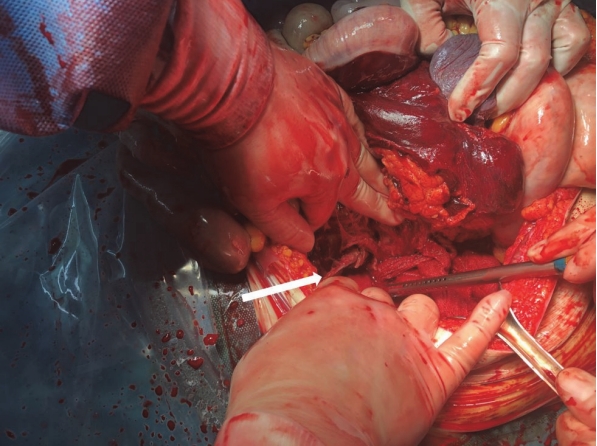
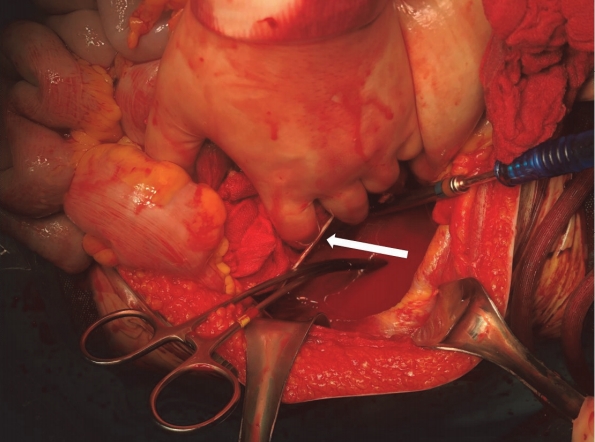
During the operation, vascular rupture from aortic bifurcation to the left common iliac artery was confirmed (Fig. 1). The REBOA catheter was found to be misplaced: It had been inserted correctly via the femoral artery, but it exited through the ruptured pore of the iliac artery (Fig. 2). We inserted the catheter back into the aorta urgently and then compressed the injured site to control bleeding; however, cardiac arrest continued. The abdomen was closed, the patient was moved to the intensive care unit, and then he was pronounced dead.
DISCUSSION
Noncompressible torso hemorrhage (NCTH) is associated with a high mortality rate (45%) and is the leading cause of death from trauma [2]. Controlling hemorrhage is therefore a key part of management. REBOA is a technique in which an inflatable balloon is temporarily inserted in aorta to increase cardiac afterload until definitive management can be performed [3]. For this reason, it has been increasingly used in trauma and prehospital care [4].
However, various complications have also been reported, such as vessel injury, distal ischemia, ischemia-reperfusion injury, and cardiovascular complications [5]. Furthermore, extreme caution is required in treating unstable pelvic fractures or potential iliofemoral vascular injuries [6].
I therefore suggest that REBOA be performed by experienced, professional medical personnel and that appropriate patient selection be considered as well.
Notes
Conflict of Interest Statement
None of authors have a conflict of interest