CASE
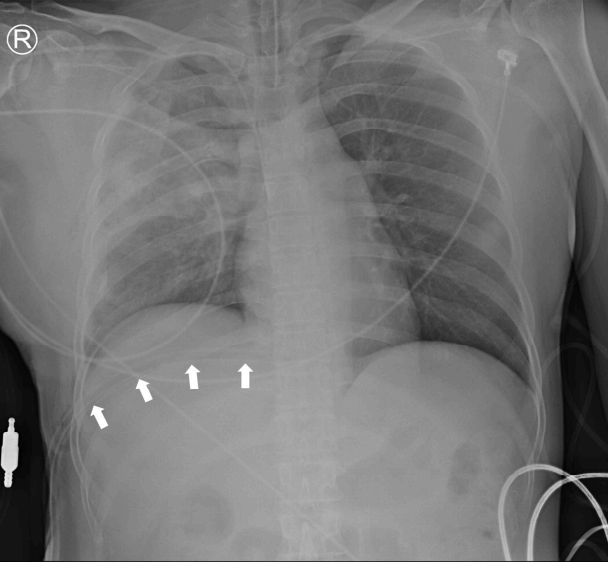
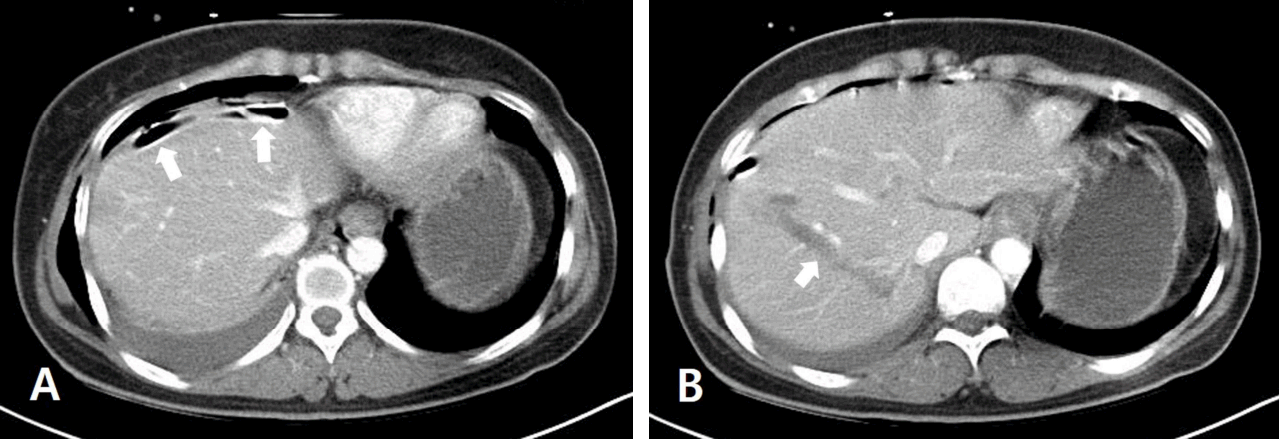
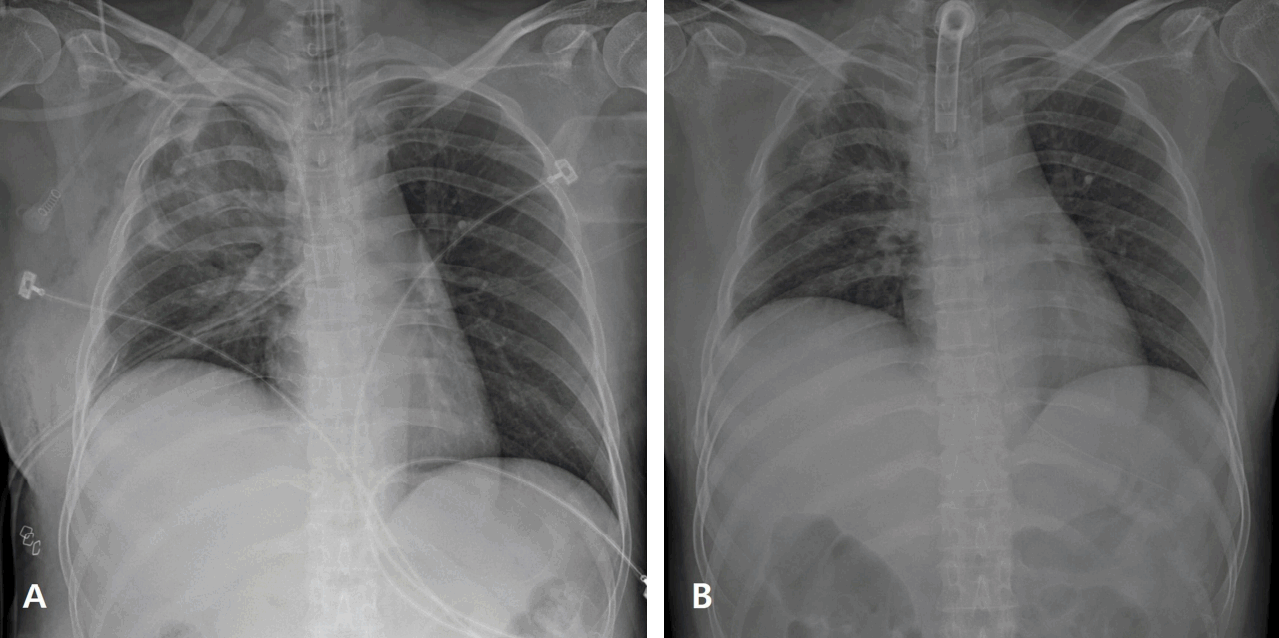
A 39-year-old woman was admitted with 8m-height falling injury by a local hospital. She underwent orotracheal intubation and right thoracostomy in the local hospital. Upon arrival, she was in a stupor with hypotension. The injury severity score was 29. The Extended Focused Assessment with Sonography for Trauma showed no intraabdominal fluid collection and no sliding sign in the right lung. Supine chest X-ray showed that the right chest tube was located in the upper right abdomen (Fig. 1). Abdomen computed tomography scan revealed a right chest tube malposition in the right subdiaphragmatic space caused penetrating hepatic injury (Fig. 2). After the chest tube reposition following removal of the chest tube in right abdomen, Supine chest X-ray showed the elevation of the right diaphragm (Fig. 3A). Mechanical ventilator was maintained for several days and weaning of ventilator was failed three times due to the difficulty of cough, excessive tracheal secretion, and right lung collapse waxed and waned. Tracheostomy was performed in hospital day 15 (Fig. 3B). As coughing was gradually improved, weaning of tracheostomy was successfully performed in hospital day 37.
DISCUSSION
Unilateral diaphragmatic paralysis may be traumatic, tumor-related, iatrogenic, or idiopathic. This may substantially decrease partial pressure of oxygen and the breathing capacity, but not intrinsically lethal [1]. Diaphragmatic paralysis is an extremely rare complication resulting from a diaphragmatic injury owing to chest tube malpositioned into the abdomen, and most of cases are reported in neonates and children [2]. Chest tube placement is a common procedure in trauma patients, as we should be fully aware of closed thoracostomy, complications like this are entirely avoidable. A typical tube thoracostomy is placed in the 4-5th interspace at the anterior axillary line and the correct position of chest tube tip is at least 2cm distant from the spine [3].